Photo from wikipedia
Bacterial bloodstream infections are of great concern globally. Of late, the emergence of drug resistant bacteria worsen the related morbidity and mortality. This study was aimed to determine the bacterial… Click to show full abstract
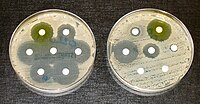
Bacterial bloodstream infections are of great concern globally. Of late, the emergence of drug resistant bacteria worsen the related morbidity and mortality. This study was aimed to determine the bacterial profile, antimicrobial susceptibility patterns, and associated factors among the blood stream infection (BSI) suspected patients attending the Arba Minch General Hospital (AMGH), southern Ethiopia, from 01 June through 31st August, 2020. A cross-sectional study was conducted among 225 BSI suspected patients. Systematic random sampling method was used to select patients. Blood culture was done to isolate bacterial pathogens. Antimicrobial susceptibility test was performed by employing the Kirby-Bauer disc diffusion method. Descriptive statistics and multivariable logistic regression analysis were done by Statistical Package for Social Service (SPSS) version 22. The rate of prevalence of bacteriologically confirmed cases was 22/225 (9.8%). Majority of BSI were caused by Gram-positive cocci, 13/22 (59.1%), particularly the isolates of S. aureus, 7/22 (31.8%) followed by Enterococci species, 4/22 (18.2%) and coagulase-negative Staphylococci (CoNS), 2/22 (9.1%). Among the Gram-negative bacteria 9/22 (41.1%), Klebsiella species 4/22 (18.2%) was the prominent one followed by Escherichia coli 2/22 (9.1%), Pseudomonas aeruginosa 2/22 (9.1%), and Enterobacter species 1/22 (4.5%). All the isolates of Gram-negative bacteria were susceptible to meropenem whereas 69.2% of the isolates of Gram-positive counterparts were susceptible to erythromycin. Slightly above two third (68.2%) of the total isolates were multidrug resistant. Insertion of a peripheral intravenous line was significantly associated with BSI [p = 0.03; Adjusted Odds Ratio = 4.82; (Confidence Interval: 1.08–21.46)]. Overall results revealed that eventhough the prevalence of BSI in Arba Minch is comparatively lower (9.8%), multidrug resistance is alarmingly on the rise, which is to be addressed through effective surveillance and control strategies.
Journal Title: Scientific Reports
Year Published: 2021
Link to full text (if available)
Share on Social Media: Sign Up to like & get
recommendations!