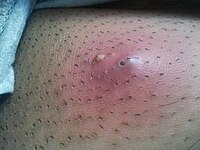
Photo from wikipedia
RATIONALE Subcutaneous and epidural abscesses following epidural injection are a serious but rare complication. Epidural abscesses are typically caused by Staphylococcus aureus bacterial infection. In this case presented here, the… Click to show full abstract
RATIONALE Subcutaneous and epidural abscesses following epidural injection are a serious but rare complication. Epidural abscesses are typically caused by Staphylococcus aureus bacterial infection. In this case presented here, the causative bacterium was Enterococcus faecalis. PATIENT CONCERNS A 67-year-old woman having chronic lower back and right leg pain with past history of 20 years of rheumatoid arthritis, diabetes mellitus, and osteoporosis (T-score: -2.7) visited the outpatient pain clinic. Magnetic resonance imaging (MRI) revealed L4-5 right central disc extrusion with inferior migration. We performed a continuous epidural block for 7 days without complications. After 10 days, she presented with worsened low back pain, erythematous skin change on the lower back, chilling, and elevated serum acute phase reactants. DIAGNOSIS The diagnosis was subsequently confirmed by MRI suggesting subcutaneous and epidural abscess. Blood and pus cultures showed the growth of E. faecalis. INTERVENTIONS Pigtail catheter drainage was performed and intravenous antibiotics (ampicillin-sulbactam) targeting E. faecalis were applied for 3 weeks. Oral antibiotics (amoxicillin/potassium clavulanate) were applied for 6 weeks after discharge. OUTCOMES At the 2-month follow-up, improvement in both the clinical condition and serum acute phase reactants levels were noted. LESSONS Epidural injection can lead to a subcutaneous abscess that is further extended into the epidural space. One of the key factors is the presence of comorbid conditions, including diabetes mellitus and prolonged steroid usage due to rheumatoid arthritis.
Journal Title: Medicine
Year Published: 2022
Link to full text (if available)
Share on Social Media: Sign Up to like & get
recommendations!